I Have Arthritis. Now What? Why Your X-Ray Doesn’t Tell the Whole Story
After years of nagging knee or back pain, you finally decide to get answers. Your doctor orders X-rays. A few days later, you’re sitting in the exam room and you hear the familiar phrase: “See that right there? That’s arthritis. That’s why you’re in pain.”
During a typical chiropractic exam, we usually take two X-ray views: one from the front and one from the side. Looking at both views together helps us better understand the shape, alignment, and condition of the spine.
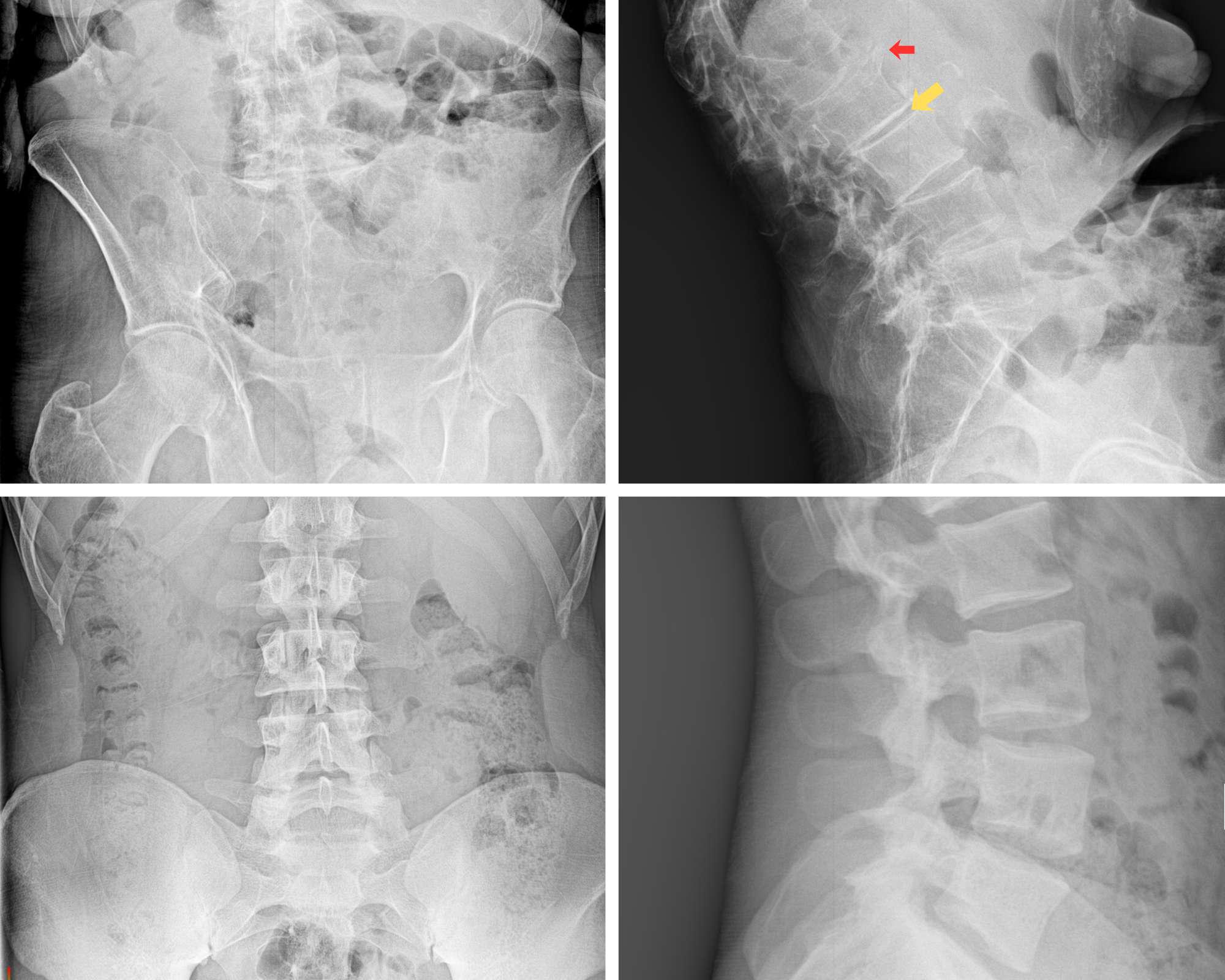
Below are two sets of spinal X-rays. The top images are from a man who is almost 90 years old. The bottom images are from a college-aged football player. Can you guess which one is in more pain?
Bone Spurs & Degenerative Disc Changes
Despite the dramatic differences seen on imaging, the college-aged football player rated his pain as a 10 out of 10, while the nearly 90-year-old reported his pain as only a 2 out of 10. This highlights a confusing truth in spine care: what shows up on an X-ray does not always match how much pain a person feels or how well they function.
The red arrow highlights an osteophyte, commonly called a bone spur, which is noticeably enlarged in this patient. In contrast, the other patient’s vertebrae appear smooth and well formed, almost like a stack of perfectly shaped marshmallows. The yellow arrow points to an area of decreased disc height, indicating thinning between the vertebrae.
That is why I never want patients to feel like their X-ray is a life sentence. Imaging can be helpful, but it is only one part of the story. The bigger question is how you move, how you feel, what you want to keep doing, and what we can do to help your body function better.
The Most Common Type of Arthritis: Osteoarthritis
Osteoarthritis (OA), sometimes called degenerative joint disease, is the most common type of arthritis. While it is often described as a simple “wear and tear” condition, that explanation is too limited. Joint degeneration is not just about what a joint looks like on imaging or how many birthdays a person has had. OA can affect the entire joint, including the cartilage, bone, ligaments, fat pad, and joint lining. It is influenced by how the joint has been used, how it has been stressed, how well it is supported, and how the body responds to those stresses over time. Understanding this makes it easier to see why osteoarthritis can develop in different ways and why symptoms can vary so much from person to person.
It is also important to remember that osteoarthritis is only one type of arthritis. Other forms, such as rheumatoid arthritis, psoriatic arthritis, gout, and ankylosing spondylitis, can have different causes and may require different types of evaluation and treatment. For this article, however, the focus will be on osteoarthritis: what it is, why it develops, and how conservative care may help manage it.
A helpful way to understand osteoarthritis is to look at its contributing factors rather than searching for one single cause. These factors can be grouped into two main categories: systemic influences, which affect the body as a whole, and mechanical influences, which affect how a specific joint is used, loaded, or stressed over time.
What Happens to a Joint With Osteoarthritis
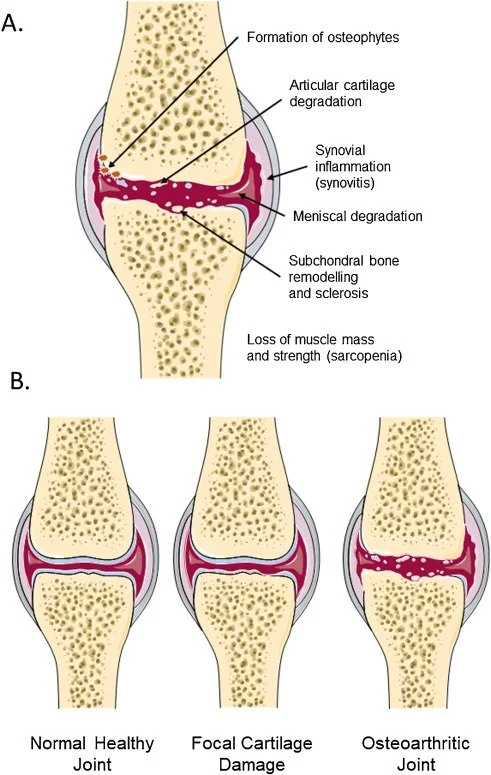
The top image (A) shows how osteoarthritis can affect the whole joint, not just the cartilage. As the condition progresses, the smooth cartilage can break down, the joint lining may become irritated, bone spurs can form, and the bone beneath the cartilage can become thicker or inflamed.
The bottom images (B) show the change from a healthy joint, to early cartilage damage, to a more advanced osteoarthritic joint.
Systemic Influences: Heredity, Gender, and Hormones
Heredity
Family history can play a role in osteoarthritis, but it does not completely decide your future. If a parent or grandparent had arthritis, that does not mean you are guaranteed to have it too. Genetics may influence joint shape, cartilage strength, bone structure, inflammation, and how your tissues respond to stress. A simple way to think about it is this: heredity may load the gun, but it does not have to pull the trigger. How you move, eat, manage old injuries, build strength, and care for your joints still matters.
Gender & Hormones
Men and women can experience osteoarthritis differently. Women are more likely than men to develop osteoarthritis, especially after age 50 and after menopause. Hormones may be part of that picture because estrogen can influence cartilage, bone, inflammation, and how joint tissues respond to stress. In men, testosterone may also matter because it is tied to muscle, bone, metabolism, and inflammation. The practical point is not that one hormone causes or prevents arthritis. The point is that joint health is connected to the whole body.
Mechanical Influences: Weight, Previous Injury, and Repetitive Stress
Extra Body Weight
Extra weight increases the load placed on weight-bearing joints, especially the knees, hips, feet, and spine. Being overweight can make the joints work harder with every step, stair, squat, or lift. Research reviews describe obesity-related osteoarthritis as being strongly tied to increased mechanical load on the lower extremity joints.
Years ago, I attended a presentation by a hip surgeon who said many people may be able to delay, or possibly avoid, hip surgery if they were able to lose weight. I asked him, “How many of your patients have actually lost weight and avoided a hip replacement?” He answered, “Zero.” That moment stuck with me. Not because weight loss is impossible, but because simple advice is not the same as an easy plan. People need realistic support, guidance, and a plan they can actually follow.
Previous Injury and Physical Work
A previous joint injury can change the way a joint moves, absorbs shock, and carries weight. This is why injuries such as ligament tears, meniscus injuries, fractures, or previous joint surgery may increase the risk of osteoarthritis later in life. One research review explains that “post-traumatic osteoarthritis develops secondary to a joint injury and accounts for 12% of all osteoarthritis.” In simple terms, an injured joint may not move or load quite the same afterward, which can place extra stress on the cartilage, bone, and surrounding tissues over time.
Certain jobs place repeated stress on the same joints over many years. Frequent kneeling, squatting, lifting, carrying, climbing, prolonged standing, or working in awkward positions may increase the risk of osteoarthritis, especially in the knees and hips. This is why someone can feel worn down in one specific joint after years of doing the same type of work.
Conservative Care for Osteoarthritis: Chiropractic, Nutrition, and Movement
Chiropractic
An osteoarthritis diagnosis can feel discouraging, but it shouldn’t be treated like the end of the road. OA may involve cartilage, bone, inflammation, muscle support, joint motion, and the way the body responds to stress over time. That means care shouldn’t only focus on the image or the diagnosis, but on how you move, function, and feel day to day.
This is where chiropractic care can be a valuable part of a conservative care plan. The goal is not to “reverse” arthritis or pretend the joint changes are not there. The goal is to help the surrounding joints and tissues move better, reduce unnecessary stress, improve comfort, and help you stay as active and independent as possible. Remember the images that were shown at the beginning of this article? Both of those patients improved significantly, despite having very different X-ray findings.
Cox Technic is a gentle, controlled form of chiropractic care that uses flexion-distraction and decompression to help reduce stress on the discs, joints, and nerves of the spine. This can be especially helpful to discuss with degenerative changes because the discs and facet joints often affect each other. When a disc loses height or becomes irritated, extra stress can shift to the facet joints in the back of the spine. Those joints may then become stiff, compressed, or arthritic, which can contribute to low back pain, stiffness, and sometimes nerve irritation.
With Cox Technic, the spine is treated in a slow, specific, and controlled way. The goal is to gently open the spinal joints, improve motion, reduce pressure around the disc and nerve openings, and decrease irritation through the facet joints. For patients with spinal arthritis, disc degeneration, stenosis, or back and leg symptoms, this lighter approach may be a good fit because it avoids a more forceful adjustment while still helping the spine move and function better. Cox-specific research has also shown clinical improvement in patients treated with Cox Flexion Distraction Decompression for knee pain, which supports the broader idea that gentle, movement-based care may help certain arthritic or painful joints function better.
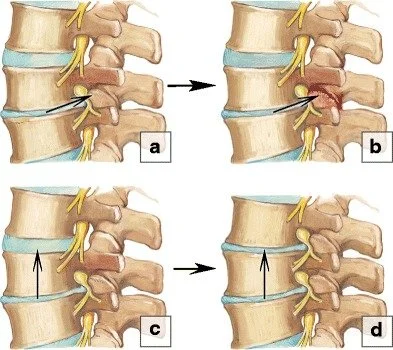
This diagram from ABCs of the Degenerative Spine shows two ways spinal degeneration can develop.
In images a-b, degeneration starts in the disc. As the disc wears down and loses height, extra stress can shift to the small joints in the back of the spine, called facet joints. Over time, those joints can become arthritic.
In images c–d, severe degeneration at one spinal level can put extra stress on the level above it. This can cause nearby areas of the spine to work harder and develop changes of their own.
Palmer Chiropractic-based techniques focus on finding areas of the spine that are not moving or functioning properly, often described in chiropractic as a subluxation. Chiropractic has evolved from D.D. Palmer’s early focus on vertebral misalignment to a broader understanding that includes anatomical, physiological, biomechanical, chemical, and biopsychosocial factors. In simple terms, a subluxation complex is an area of the spine or joint system that is not moving or functioning properly and may affect the nervous system and the body’s ability to adapt.
Palmer-style adjustments are designed to restore better motion to those joints, reduce stress on the surrounding discs, muscles, and nerves, and help the body move more comfortably. The goal is not to erase arthritis or remove bone spurs, but to improve function, reduce irritation, and help patients stay active.
Most people don’t come into the Studio because they want a perfect X-ray. They come in because they want to walk easier, sleep better, work without constantly thinking about their back or knee, and keep doing the things that make life feel normal.
Nutrition
When dealing with osteoarthritis, one goal is to keep the body’s inflammatory load as low as possible. Dr. Barry Sears, known for his work on the Zone Diet, often discusses omega-3 fish oil as a tool for helping the body “resolve” inflammation, especially because EPA and DHA are used to produce inflammation-resolving compounds. This does not mean fish oil cures arthritis, but it may help support a healthier inflammatory response.
Food matters, too. A diet built around protein, colorful vegetables, fruit, healthy fats, and fewer processed foods will help reduce inflammatory stress on the body. Limiting added sugar, refined carbohydrates, fried foods, processed foods, and seed oils while adding more omega-3-rich options such as salmon, sardines, or high-quality fish oil can be a simple place to start. For arthritis, the goal is not perfection. The goal is to give your joints and tissues a better environment to function in. Start with a few simple changes.
A Sweet Treat, Best Enjoyed Occasionally
There is nothing wrong with enjoying a donut once in a while, but it is best thought of as a treat rather than a routine part of an osteoarthritis-friendly diet. Foods like donuts are typically high in added sugar and refined flour, so they are better enjoyed occasionally while focusing more often on foods that support overall health.
Yoga, Physical Therapy and Strength Training
Movement can feel intimidating when a joint is already stiff, sore, or unstable. That is why gentle, guided movement matters. Yoga can be one of the best first steps because it gives you a low-pressure way to improve mobility, balance, breathing, body awareness, and confidence without trying to keep up with anyone else.
Physical therapy can help take that progress further by identifying specific weaknesses, limitations, or movement patterns that need more attention. Strength training also matters because stronger muscles give arthritic joints better support. The goal is not to train like an athlete, but to build enough strength and stability to make daily life easier.
Get Ahead of Arthritis Before It Gets Ahead of You
This article was written for people dealing with osteoarthritis, but the bigger message applies to everyone: do not wait until pain or stiffness becomes a major problem before taking care of yourself. Arthritis is often a sign that the body needs better movement, better support, and a healthier internal environment. The earlier you address those areas, the better chance you have of staying active, mobile, and independent. Think about it like this: do you want to stay in your own home as you get older? Do you want to climb stairs, carry groceries, get out of a chair, play with your grandkids, and keep doing the things you enjoy? Then your spine, joints, muscles, and overall health need attention now, not later.
Start with the basics. Find a chiropractor who can evaluate your spine and joints and help you determine the best treatment plan for your body. Schedule a visit with a physical therapist to learn your limitations, build strength safely, and improve how you move. As you build confidence, continue strengthening with simple weights at home or consider joining a gym to keep gaining muscle and stability. Consider adding yoga as a gentle way to improve mobility, balance, breathing, and body awareness while keeping your joints moving in a controlled way. And lastly, begin eating in a way that supports lower inflammation, and consider reading Anti-Inflammation Zone by Dr. Barry Sears to better understand how food choices may influence your body’s inflammatory response.
At our Studio in Weyauwega, we help patients understand what their X-rays show, what those findings actually mean, and what conservative options may help them move and function better. The goal is simple: get ahead of arthritis before it gets ahead of you.
In good health,
Dr. Joshua A. Belville
Featured image for social media content courtesy of: Adapted from Damerau et al., Frontiers in Immunology 2024, “Fibrotic pathways and fibroblast-like synoviocyte phenotypes in osteoarthritis,” Figure 1. Licensed under CC BY 4.0. doi:10.3389/fimmu.2024.1385006.